My Gut Feeling About Gluten: Is Gluten Sensitivity Real?
Okay, let’s talk gluten. As someone who’s navigated a minefield of dietary restrictions (hello, dairy intolerance!), I get how confusing the whole gluten thing can be. You hear about Celiac Disease, gluten intolerance, gluten sensitivity… it’s enough to make your head spin! So, is gluten sensitivity real? That’s what we’re diving into today. I’m going to share what I’ve learned, separate fact from fiction, and help you understand the difference between gluten sensitivity and Celiac Disease.
Table of Contents
- My Gut Feeling About Gluten: Is Gluten Sensitivity Real?
- What is Gluten, Anyway?
- Celiac Disease: An Autoimmune Reaction
- Key characteristics of Celiac Disease:
- Non-Celiac Gluten Sensitivity (NCGS): The Mystery Illness
- Why the skepticism?
- My Own (Potentially Gluten-Related) Story
- The Verdict: So, is Gluten Sensitivity Real?
- Distinguishing Between Gluten Sensitivity and Celiac Disease
- What To Do If You Suspect Gluten Sensitivity: A Step-by-Step Guide
- Navigating the Gluten-Free Aisle
- Final Thoughts: Listen to Your Body
For years, I brushed it off. “Oh, another fad diet,” I thought. But then, more and more friends started talking about how much better they felt when they cut gluten. And honestly, I started paying closer attention to how I felt after eating certain things. That bloated, sluggish feeling after a big plate of pasta? Yeah, I started wondering. Let’s get into it, shall we?
What is Gluten, Anyway?
Before we go any further, let’s get clear on what gluten actually *is*. Gluten is a family of proteins found in grains like wheat, barley, and rye. It’s what gives bread its chewy texture. Think of it as the “glue” that holds things together. (See what I did there?).
Celiac Disease: An Autoimmune Reaction
Celiac Disease is an autoimmune disorder. When someone with Celiac Disease eats gluten, their immune system attacks their small intestine. This can lead to serious damage over time, hindering the body’s ability to absorb nutrients. Symptoms can range from digestive issues to fatigue, anemia, and even neurological problems.
It’s not just a tummy ache; it’s a serious condition that requires a lifelong gluten-free diet. It can be tested for via blood tests and endoscopy. If you suspect you have Celiac Disease, please see a doctor to get an accurate diagnosis. You can’t just cut out gluten and assume all is well. Getting tested while still consuming gluten is key to accurate results.
Key characteristics of Celiac Disease:
- It’s an autoimmune disease.
- Causes damage to the small intestine.
- Diagnosed via blood tests and endoscopy.
- Requires a strict, lifelong gluten-free diet.
Non-Celiac Gluten Sensitivity (NCGS): The Mystery Illness
Okay, now we get to the murky waters of Non-Celiac Gluten Sensitivity, or NCGS. This is where the debate really heats up. People with NCGS experience symptoms similar to those with Celiac Disease after eating gluten, but they don’t have the same antibodies or intestinal damage. Their Celiac Disease test come back negative.
Symptoms can include:
- Bloating
- Abdominal pain
- Fatigue
- Headaches
- Brain fog
- Joint pain
The thing is, there’s no definitive test for NCGS. It’s often diagnosed by exclusion – meaning, after ruling out Celiac Disease and wheat allergy, if someone feels better on a gluten-free diet, they might be diagnosed with NCGS. This is why some doctors remain skeptical.
Why the skepticism?
A few reasons:
- No clear diagnostic marker: Unlike Celiac Disease, there’s no blood test or biopsy that can definitively diagnose NCGS.
- Placebo effect: Some studies suggest that the perceived improvement on a gluten-free diet might be due to the placebo effect.
- Other culprits: Gluten isn’t the only potential offender in wheat and other grains. FODMAPs (fermentable oligosaccharides, disaccharides, monosaccharides, and polyols), for example, can cause similar symptoms in some people.
My Own (Potentially Gluten-Related) Story
So, here’s my story. Remember that pasta I mentioned? Well, for a while, I just assumed I was getting older and that my metabolism was slowing down. But then I started experimenting. I cut out gluten for a week, and lo and behold, the bloating decreased, and I felt lighter. Was it a miracle cure? No. But it was enough to make me pay closer attention.
I wouldn’t self-diagnose, and I always recommend talking with a doctor and/or nutritionist to see if getting tested for any conditions like Celiac Disease is right for you. I also avoid processed gluten-free junk food, because let’s be real, that stuff’s not healthy. Focus on naturally gluten-free foods like fruits, vegetables, lean proteins, and gluten-free grains like quinoa and rice.
The Verdict: So, is Gluten Sensitivity Real?
The short answer? It’s complicated. While some doctors still have their reservations, many healthcare professionals acknowledge that some people genuinely experience adverse reactions to gluten, even if they don’t have Celiac Disease. Whether it’s truly a sensitivity to gluten itself or to other components of wheat and related grains is still up for debate.
Distinguishing Between Gluten Sensitivity and Celiac Disease
Understanding the difference between gluten sensitivity and Celiac Disease is crucial for managing your health effectively. Here’s a comparison table:
| Feature | Celiac Disease | Gluten Sensitivity |
|---|---|---|
| Immune Response | Autoimmune reaction | No autoimmune reaction |
| Intestinal Damage | Yes | No |
| Diagnostic Tests | Blood tests, endoscopy | No specific test |
| Treatment | Strict gluten-free diet | Gluten-free diet (may be less strict) |
| Long-Term Effects | Malnutrition, increased risk of other autoimmune diseases | Less severe, primarily symptom management |
What To Do If You Suspect Gluten Sensitivity: A Step-by-Step Guide
If you think you might be gluten sensitive, here’s my suggested plan of action:
- Consult a Doctor: The very first step is consulting a healthcare professional. Discuss your symptoms and concerns. Rule out Celiac Disease and wheat allergy with appropriate testing.
- Keep a Food Diary: Track everything you eat and how you feel afterward. Note any symptoms that arise after consuming gluten-containing foods. This can help you identify patterns and triggers.
- Elimination Diet: Under the guidance of a healthcare professional or registered dietitian, try a gluten-free elimination diet. Completely remove gluten from your diet for a few weeks.
- Reintroduction Phase: After the elimination period, slowly reintroduce gluten-containing foods, one at a time. Pay close attention to how you feel after each reintroduction. This will help you determine if gluten is indeed the culprit.
- Monitor Symptoms: Continue monitoring your symptoms throughout the process. Note any changes in your digestion, energy levels, skin, or overall well-being.
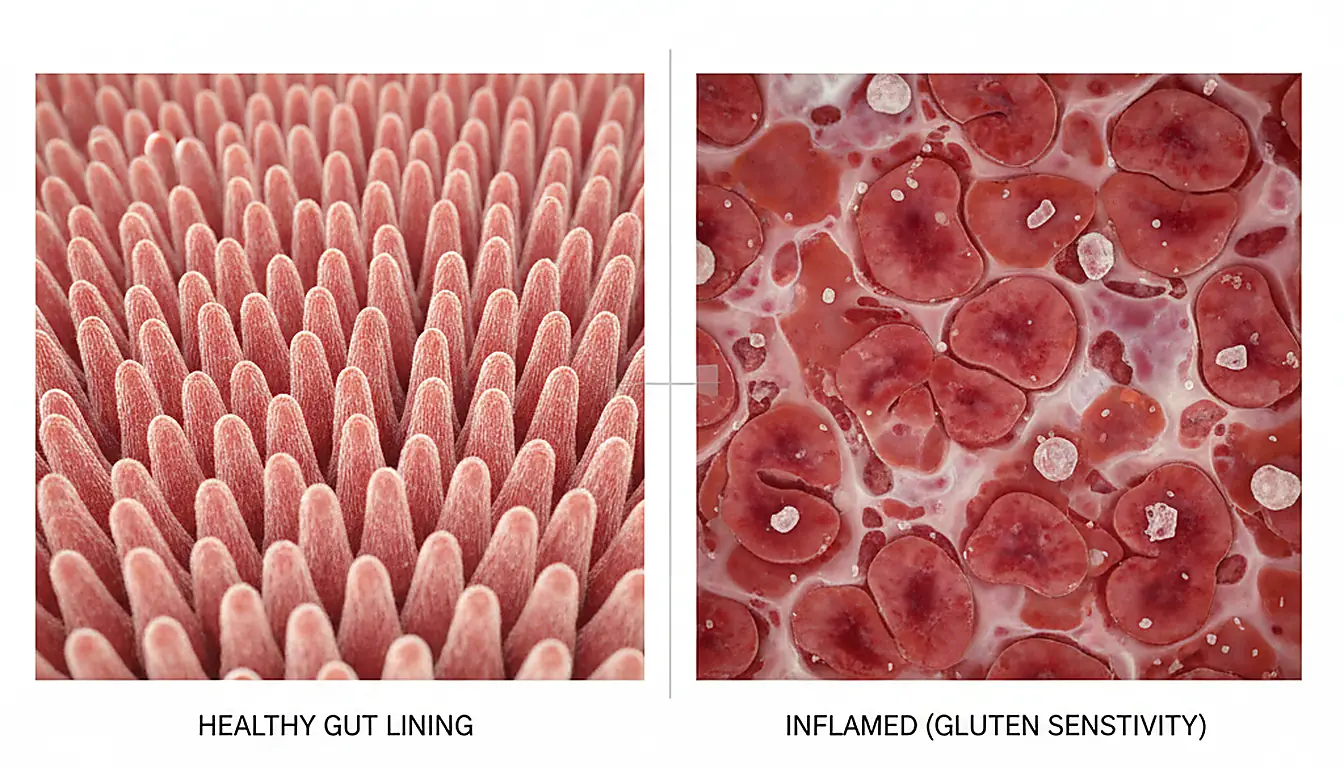
If you’re like me, you’ll appreciate this detail.
Navigating the Gluten-Free Aisle
If you do decide to go gluten-free, be aware that many processed gluten-free products are high in sugar and unhealthy fats. Focus on whole, unprocessed foods like fruits, vegetables, lean proteins, and gluten-free grains like quinoa, brown rice, and oats (make sure they’re certified gluten-free to avoid cross-contamination).
Final Thoughts: Listen to Your Body
Ultimately, the most important thing is to listen to your body. If you feel better on a gluten-free diet, that’s valuable information. Don’t let anyone dismiss your experience. At the same time, be mindful of potential nutrient deficiencies and ensure you’re getting a balanced diet. Consult with a registered dietitian to create a personalized meal plan that meets your needs.
Whether it’s Celiac Disease, Non-Celiac Gluten Sensitivity, or something else entirely, understanding how food affects your body is essential for your overall well-being. And that, my friends, is something worth exploring!
FAQ About Gluten Sensitivity and Celiac Disease
-
Question: What are the main differences between Celiac Disease and gluten sensitivity?
Answer: Celiac Disease is an autoimmune disorder where gluten triggers an immune response that damages the small intestine. Gluten sensitivity (NCGS) causes similar symptoms but without the autoimmune response or intestinal damage. The key differences lie in the immune reaction and the presence or absence of intestinal damage.
-
Question: How is gluten sensitivity diagnosed?
Answer: Gluten sensitivity is typically diagnosed by excluding Celiac Disease and wheat allergy. If someone experiences symptoms after consuming gluten and feels better on a gluten-free diet, they may be diagnosed with NCGS. There isn’t a specific test for gluten sensitivity.
-
Question: Is a gluten-free diet necessary for someone with gluten sensitivity?
Answer: A gluten-free diet is generally recommended for managing gluten sensitivity. It involves avoiding foods containing wheat, barley, and rye. However, the strictness of the diet may vary from person to person based on their symptom severity.
-
Question: Can gluten sensitivity lead to long-term health issues?
Answer: Gluten sensitivity primarily leads to symptom management, while Celiac Disease can cause malnutrition and increase the risk of other autoimmune diseases if left unmanaged.
-
Question: What should I do if I suspect I have gluten sensitivity?
Answer: If you suspect gluten sensitivity, consult a doctor to rule out Celiac Disease and wheat allergy. Keep a food diary to track your symptoms and consider an elimination diet under professional guidance. Monitor how you feel as you reintroduce gluten-containing foods to determine if gluten is causing your symptoms.
Frequently Asked Questions
What are the main differences between Celiac Disease and gluten sensitivity?
Celiac Disease is an autoimmune disorder where gluten triggers an immune response that damages the small intestine. Gluten sensitivity (NCGS) causes similar symptoms but without the autoimmune response or intestinal damage. The key differences lie in the immune reaction and the presence or absence of intestinal damage.
How is gluten sensitivity diagnosed?
Gluten sensitivity is typically diagnosed by excluding Celiac Disease and wheat allergy. If someone experiences symptoms after consuming gluten and feels better on a gluten-free diet, they may be diagnosed with NCGS. There isn’t a specific test for gluten sensitivity.
Is a gluten-free diet necessary for someone with gluten sensitivity?
A gluten-free diet is generally recommended for managing gluten sensitivity. It involves avoiding foods containing wheat, barley, and rye. However, the strictness of the diet may vary from person to person based on their symptom severity.
Can gluten sensitivity lead to long-term health issues?
Gluten sensitivity primarily leads to symptom management, while Celiac Disease can cause malnutrition and increase the risk of other autoimmune diseases if left unmanaged.
What should I do if I suspect I have gluten sensitivity?
If you suspect gluten sensitivity, consult a doctor to rule out Celiac Disease and wheat allergy. Keep a food diary to track your symptoms and consider an elimination diet under professional guidance. Monitor how you feel as you reintroduce gluten-containing foods to determine if gluten is causing your symptoms.
Key Takeaways
- My Gut Feeling About Gluten: Is Gluten Sensitivity Real?
- What is Gluten, Anyway?
- Celiac Disease: An Autoimmune Reaction
- Key characteristics of Celiac Disease
- Non-Celiac Gluten Sensitivity (NCGS): The Mystery Illness




